The magic of deep brain stimulation has yet to be lost on neurosurgeon Associate Professor Terry Coyne and neurologist Professor Peter Silburn, even after having performed a thousand of the delicate operations.
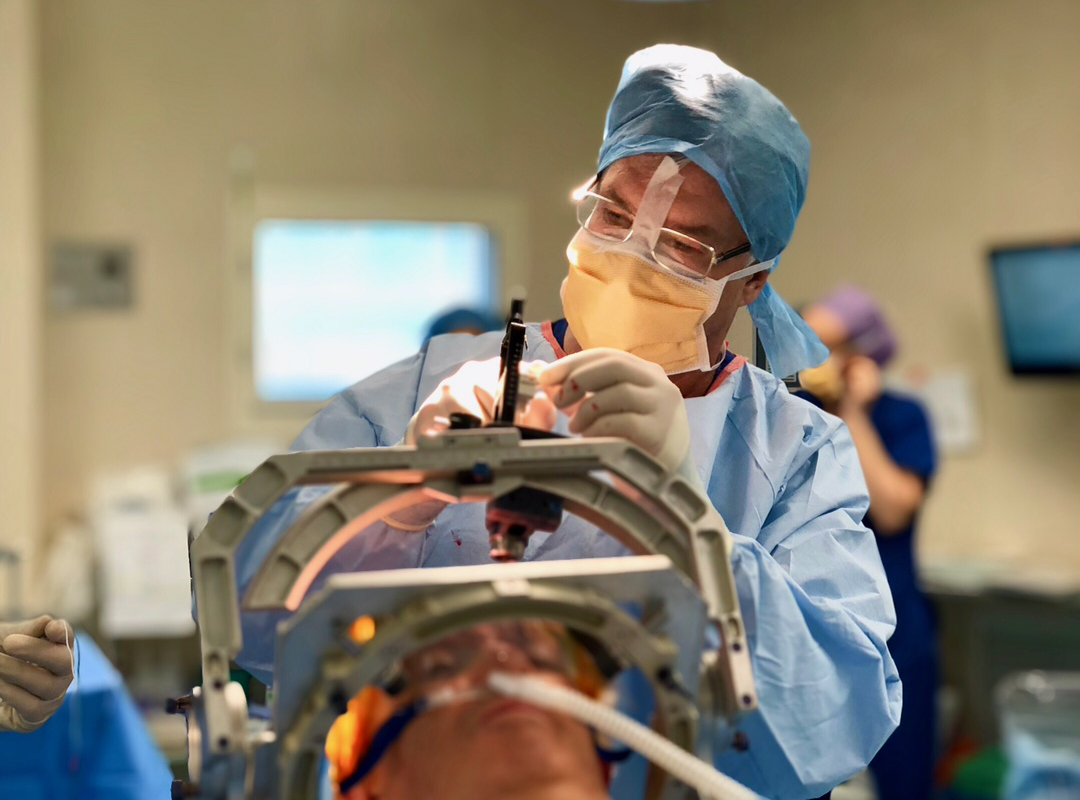
It’s the kind of moment that can never get old. Within the still focus of theatre, the surgery team watches as Associate Professor Coyne inserts a long, extremely thin electrode – around 2mm – into the patient’s brain. The effect is almost instantaneous. Tremors and tics that have plagued patients for years disappear in moments. The patients – who are awake during the surgery – see their lives literally change before their eyes.
Associate Professor Coyne has over 30 years of experience as a clinical neurosurgeon. With Professor Silburn, the pair has trained over 85% of Australian deep brain stimulation teams, recently performing their 1000th DBS surgery. Professor Silburn was awarded the Member of the Order of Australia (AM) in 2013, and A/Professor Coyne was awarded the Medal of the Order of Australia (OAM) in 2017, both for their work in deep brain stimulation.
The globally renowned duo have been involved in training Asia Pacific deep brain stimulation teams and have supervised the first deep brain stimulation surgeries in locations such as Jakarta, Indonesia and Shenzhen, China.
What is deep brain stimulation?
Deep brain stimulation is a surgical procedure used to manage the symptoms of conditions such as Parkinson’s disease. Electrodes are inserted into very specific areas of the patient’s brain to stimulate brain activity within those regions and stop symptoms, such as tremors, rigidity, freezing, and slowness.
While DBS is not a cure for Parkinson’s, it offers relief from the disease and allows people to regain control of their lives.
“What we offer people is independence and an improved quality of life,” A/Professor Coyne said.
“It can reverse years of debilitating symptoms almost instantly. You can see the relief on people’s faces as they realise their hands have stopped shaking for the first time in years, and that’s the most rewarding part. That’s what makes it all worth it.”
The surgery is inconceivably intricate, with the millimetres-thick electrodes needing to be placed in precise spots to avoid stimulating the wrong neurons. Communication between the neurologist (Professor Silburn) and the neurosurgeon (A/Professor Coyne) is critical in ensuring this process runs smoothly.
During insertion, the patient is awake to ensure the correct areas are being stimulated and the brain is not being damaged. The brain itself has no pain receptors, so the patient does not feel the insertion.
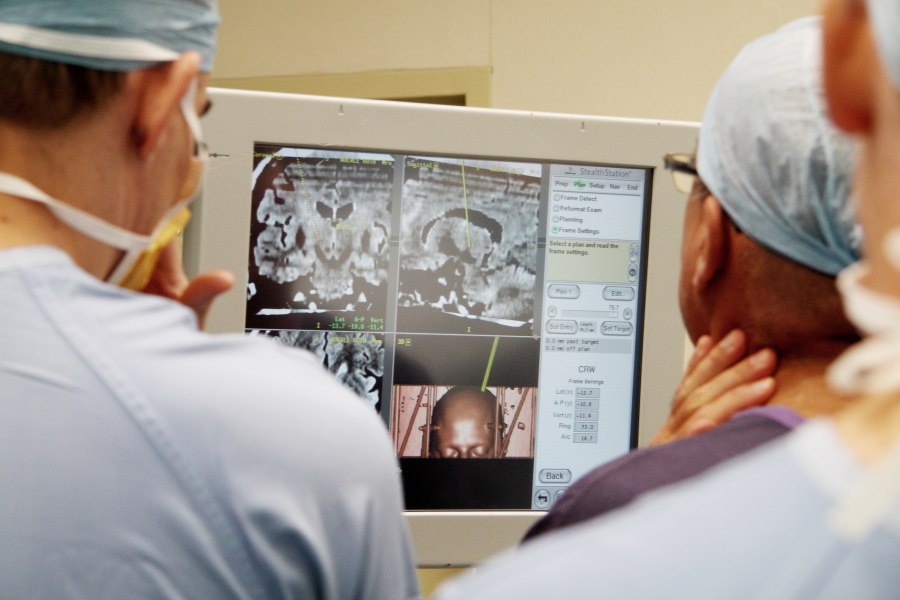
“It’s a very intense moment, when you’re inserting the electrode,” A/Professor Coyne said. “You have this tiny area that you can’t see by eye, so you’re relying on imagery, recordings of the brains electric activity and patient’s response to electric stimulation during the surgery.”
“The actual insertion needs to be quick, so you need to be confident in what you’re doing.”
Clinic meets lab to better understand the brain
While A/Professor Coyne has his own private neurosurgery practice, he and Professor Silburn are also part of the Asia-Pacific Centre for Neuromodulation (APCN), a joint initiative between the Queensland Brain Institute at The University of Queensland and St Andrew’s War Memorial Hospital.
Data from the deep brain stimulation surgeries is being used in research at the Centre to improve the process and understanding of DBS, and the brain as a whole.
“Working as both a clinician and a researcher, I have the opportunity to use my knowledge and experiences as a neurosurgeon to learn more about the brain as a researcher,” A/Professor Coyne said.
“The data we collect from electrophysiological recordings in patients undergoing DBS reveals what exactly is happening in the brain in disorders such as Parkinson’s disease.”
“Understanding the precise mechanisms of what goes wrong in the brain in these diseases may contribute to finding a cure in the future,” he said.



